The Critical Status Quo
“The initiation of ventilation in the delivery room is one of the most important but least controlled interventions a preterm infant will face. Tidal volumes (VT) used in the neonatal intensive care unit (NICU) are carefully measured and adjusted. However, the Volumes that an infant receives (in the delivery room) during resuscitation are usually unmonitored and highly variable…”
“Inappropriate VTs delivered to preterm infants during respiratory support substantially increase the risk of injury and inflammation to the lungs and brain. These may cause cerebral blood flow instability and initiate a cerebral inflammatory cascade. The two pathways increase the risk of brain injury and potential life-long adverse neurodevelopmental outcomes” Samantha K. Barton, Mary Tolcos, Suzie L. Miller, Charles C. Roehr, Georg M. Schmölzer, Peter G. Davis, Timothy J. M. Moss, Domenic A. LaRosa, Stuart B. Hooper and Graeme R. Polglase. ‘Unravelling the Links Between the Initiation of Ventilation and Brain Injury in Preterm Infants’ Frontiers in Pediatrics 10 November 2015 https://www.frontiersin.org/articles/10.3389/fped.2015.00097/full http://loop-impact.frontiersin.org/impact/article/165314#totalviews/views
“Despite the great advances in neonatal care over almost 50 years, the rates of Brochopulmonary Dysplasia (BPD) are not decreased and may even have risen.”Tae-Jung Sung. Korean J Pediatr. ‘Bronchopulmonary dysplasia; what should we do to improve its outcomes?’ https://www.kjp.or.kr/journal/view.php?doi=10.3345/kjp.2019.0017
“Despite major improvements in the care and outcome of extremely preterm infants over the last few decades, BPD (especially severe BPD) remains a challenging disease to treat and presents several challenges to clinicians. Its effects can be seen not only in the lungs of these infants but also in many other organ systems. BPD is a risk factor for the development of Cerebral Palsy (CP), with a significant increase in rates of CP in patients with severe BPD.”
“Ten million newborns worldwide each year need resuscitation assistance. More than 1 million babies die annually from complications of birth asphyxia” Thomas E Wiswell MD. ’Neonatal Resuscitation’ Respiratory Care March 2003, 48 (3) 288-295 http://rc.rcjournal.com/content/48/3/288
“Neonatal chronic lung disease (more recently termed Brochopulmonary Dysplasia/BPD) is the major long-term pulmonary complication of preterm birth affecting about 20% of infants who need respiratory assistance” (>2 million) Sweet, David G, Halliday, Henry ‘Treatments in Respiratory Medicine.’ 4(5):347-359, 2005. https://link.springer.com/article/10.2165%2F00151829-200504050-00006
“Reducing the rate of BPD and identifying new specific targeted therapies for established BPD remains one of the biggest challenges for neonatologists and pediatric pulmonologists.” Frances Flanagan and Anita Bhandari.‘Bronchopulmonary Dysplasia and Cerebral Palsy’. Springer Nature Switzerland AG 2019 Cerebral Palsy. https://doi.org/10.1007/978-3-319-50592-3_67-1
Whereas current devices use pressure in an attempt to deliver a safe volume, the NextStep™ uses an operator pre-set and microprocessor-controlled miniature servomotor to deliver a patient-specific volume, within 10% of Operator pre-set target, irrespective of compliance change throughout the resuscitation process.
Current Neonatal Resuscitators
Multiple companies make the three types of Current Neonatal Resuscitators, all pressure-driven. Examples shown below:

A. Self-Inflating Bag
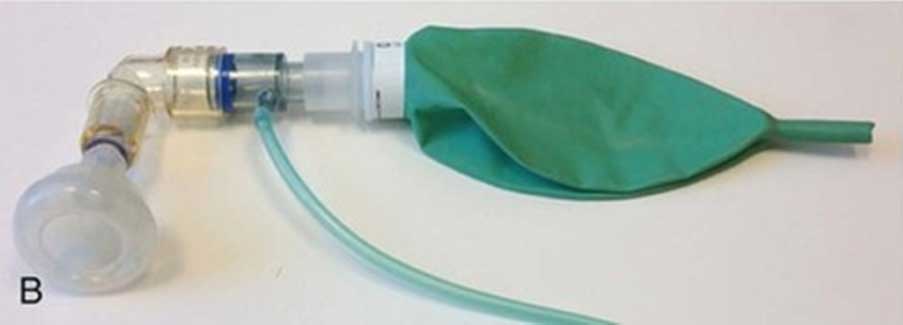
B. Flow-Inflating Bag
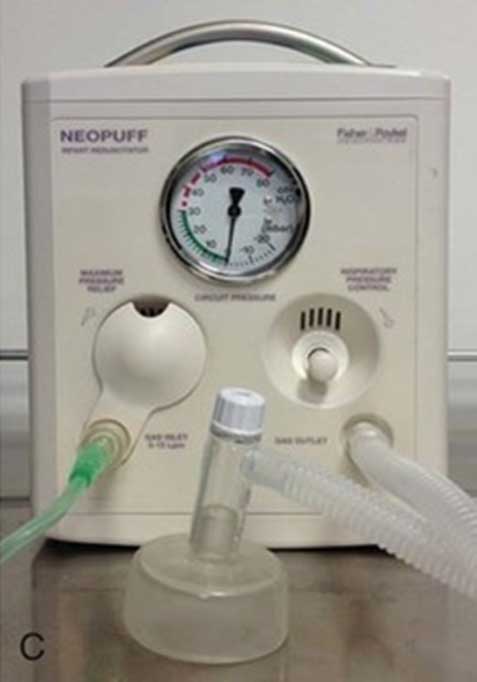
C. T-Piece
Photos: ‘Goldsmith’s Assisted Ventilation of the Neonate: An Evidence-Based Approach to Newborn Respiratory Care. P Martin Keszler & K. Suresh Gautham 7th edit P.158
Current Neonatal Resuscitators were developed in the 1900’s when excessive pressure was thought to be the primary cause of lung injury (Barotrauma). They are pressure driven and accordingly impaired in their ability to deliver controlled, safe volume as the Newborn’s lung compliance increases during transition to extrauterine life, from fluid-filled to air-filled.
Multiple studies have since proven the primary cause of lung and brain injury to be excessive Volume (Volutrauma) and life-long Respiratory and Neurological impairment, including Cerebral Palsy.
These injuries impact over 2M Newborns annually and can be sustained in the Delivery Room (DR) prior to admission to the Neonatal Intensive Care Unit (NICU). Additionally over 1M die.
More Problems with current Neonatal Resuscitators
Self-Inflating Bag types:
“A controlled bench test was undertaken to determine the performance variability among a range of neonatal self-inflating bags (SIB) compliant with current International Standards Organisation. No (previous) systematic study has evaluated variance in different models of neonatal SIB.”
“RESULTS: Ten out of the 20 models of SIB failed our testing methodology. Two models could not provide safe minimum tidal volumes (2.5-5 mL); six models exceeded safety inflation pressure limit >45 cm H2O, representing 6% of their inflations; five models had excessive coefficient of variation (>30% averaged across compression distances) and three models did not deliver inflation volumes >2.5 mL until approximately 50% of maximum bag compression distance was reached. The study also found significant intra-batch variability and forward leakage.”
“CONCLUSION: Compliance of SIBs with ISO standards may not guarantee acceptable or safe performance to resuscitate newborn infants.” Tracy MB, Halliday R, Tracy SK, Hinder MK. ‘Newborn self-inflating manual resuscitators: precision robotic testing of safety and reliability.’ Arch Dis Child Fetal Neonatal Ed. 2018 Oct 18. pii: fetalneonatal-2018-315391. doi: 10.1136/archdischild-2018-315391. https://fn.bmj.com/content/fetalneonatal/early/2018/10/18/archdischild-2018-315391.full.pdf
T-Piece types:
“The T-piece resuscitator (TPR) has seen increased use as a primary resuscitation device with newborns.”
”Results show important variation in delivered ventilation from set values due to inherent TPR device design characteristics with a range of lung compliances expected at birth. Significant differences were seen in tidal volumes across devices particularly at higher Compliance.
Device-generated inadvertent PEEP and over delivery of PIP may be clinically deleterious for term and preterm newborns or infants with larger Compliance during resuscitation.” Murray Hinder, Alistair McEwan, Thomas Drevhammer, Snorri Donaldson, Mark Brian Tracy. ‘T-piece Resuscitators: How do they compare?’ May 2018 BMJ Archives of Disease in Childhood – Fetal and Neonatal Edition https://fn.bmj.com/content/104/2/F122
Fighting Physics
Using pressure-driven resuscitators in an attempt to deliver safe, controlled volume throughout increases in lung compliance as the New-born’s lungs transition, is effectively Fighting Physics.
Physics dictates that any Pressure-Driven Neonatal Resuscitator must deliver increasing volume as the Newborn’s lung compliance increases.
The equation of compliance states that lung Compliance = change in Volume/change in Pressure. Jay P. Desai; Fady Moustarah ‘Pulmonary Compliance’
https://www.ncbi.nlm.nih.gov/books/NBK538324
From this we see that when Compliance increases (i.e. lung becomes softer) and Pressure remains constant, Volume must increase.
“Since intubation and positive pressure ventilation were first recommended by Flagg in North America in 1928, and by Blaikley and Gibberd at Guy’s Hospital in 1935, a pattern of resuscitation has evolved based on extrapolation and assumption rather than on clinical measurement. There can be few areas of medicine in which the potential benefit is so great, but which have been subjected to so little evaluation” Milner, A. D. ‘Resuscitation of the Newborn’ Arch.Dis.Child 1991;66:66-69
“Despite advances in neonatal intensive care, more than half of surviving infants born Extremely Preterm (EP; <28 weeks’ gestation) develop bronchopulmonary dysplasia (BPD).
Prevention of BPD is critical because of its associated mortality and morbidity, including adverse neurodevelopmental outcomes and respiratory health in later childhood and beyond.” Louise S Owen MD123 Brett J Manley PhD123 Kate A Hodgson MBBS (Hons)12 Calum T Roberts PhD456 ‘Impact of early respiratory care for extremely preterm infants’ https://www.sciencedirect.com/science/article/abs/pii/S0146000521000926
“Intraventricular haemorrhage (IVH) and bronchopulmonary dysplasia (BPD) are major complications of premature birth.”
“Reducing the rate of BPD and identifying new specific targeted therapies for established BPD remains one of the biggest challenges for neonatologists and pediatric pulmonologists.” Frances Flanagan Anita Bhandari. ‘Bronchopulmonary Dysplasia and Cerebral Palsy’. Springer Nature Switzerland AG 2019 Cerebral Palsy. https://doi.org/10.1007/978-3-319-50592-3_67-1
“Avoidance of high tidal volumes and hypocarbia in the delivery suite might reduce Intraventricular Haemorrhage (IVH) development.” Pahuja A, Hunt K, Murthy V, Bhat P, Bhat R, Milner AD, Greenough A. ‘Relationship of resuscitation, respiratory function monitoring data and outcomes in preterm infants.’ Eur J Pediatr. 2018 Nov;177(11):1617-1624.https://link.springer.com/article/10.1007/s00431-018-3222-y
”Faced with level 1 evidence of important benefits of Volume Targeted Ventilation/VTV (in the Neonatal Intensive Care Unit/ NICU), it is hard to justify continuing to expose infants to pressure-controlled ventilation (in the Delivery Room/DR) . The way forward is for us to be willing to abandon our comfort zone and embrace the paradigm shift that VTV represents.” Keszler M. ‘Volume-targeted ventilation: One size does not fit all. Evidence-based recommendations for successful use.’ Arch Dis Child Feta Neonatal Ed 2018; 0:F1–F5.
https://relaped.com/wp-content/uploads/2018/08/Volume-targeted-ventilation.pdf
Volume Targeted Ventilation (VTV) is available on most modern neonatal ventilators, and its use is supported by physiologic considerations and human trials showing improvement in several important clinical outcomes with no adverse effects compared with Pressure Limited Ventilation (PLV). Volume Targeted Ventilation (VTV) should be the default neonatal ventilation mode.” Belteki G, Morley CJ. ‘Volume-Targeted Ventilation.’ Clinics in Perinatology. 2021 Dec 1;48(4):825-41. https://www.journals.elsevier.com/clinics-in-perinatology/recent-articles


